Meniere's Disease
What is it and what causes it?
What is Meniere’s disease?
Meniere’s disease affects the inner part of the ear, which is the centre of hearing and balance. During an attack, the person experiences vertigo – a sensation that they or the world around them is moving. They can feel dizzy and sick, experience hearing loss and develop a hissing or roaring sound (tinnitus). The ears may also feel blocked or full. Typically, only one ear is affected initially; however, over time both ears may become involved.
Meniere’s disease may develop slowly over time, with a gradual loss of hearing, or suddenly with a vertigo attack. Attacks can last from 10 minutes to several hours.
After an attack, the person may experience some hearing loss and feel unsteady. As the disease progresses, the episodes of vertigo often become less frequent and the hearing loss can become more severe.
Meniere’s diseases is very common (more than 500,000 cases per year in Australia) and has higher prevalence in females and often affects people in the 18-35 age group.
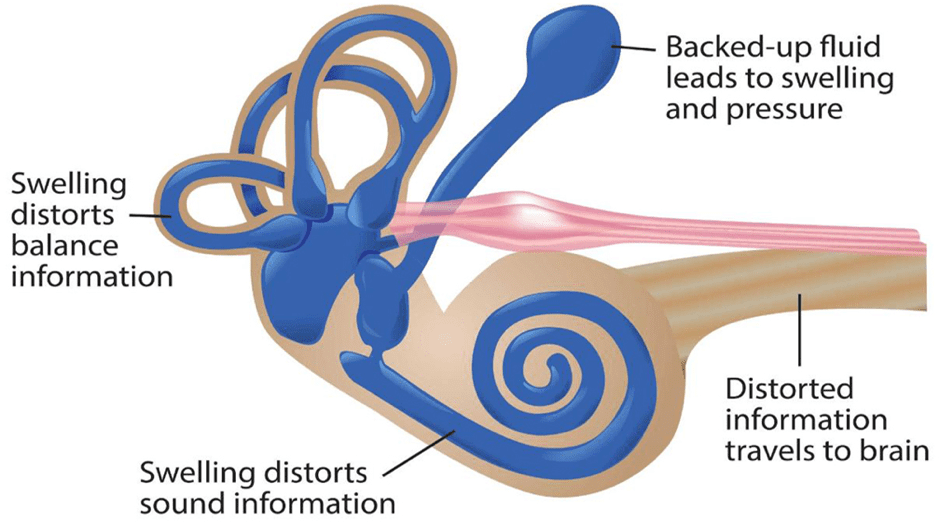
The inner ear – balance and hearing
The inner ear contains a series of canals filled with fluid. These canals are at different angles. When your head is moved, the rolling of the fluid inside these canals tells your brain exactly how far, how fast and in what direction your head is moving. Information from these canals is passed along to the brain via the vestibular (balance) nerve. If your brain knows the position of the head, it can work out the position of the rest of your body.
The cochlea is the snail-shaped hearing organ in your inner ear, which is also filled with fluid. This fluid moves in response to sounds. Messages are passed along the hearing nerve to the brain to tell you what you are hearing. The build-up of fluid associated with Meniere’s disease disturbs the hearing nerve endings, causing hearing fluctuation and eventually permanent damage.
Causes of Meniere’s disease
The cause of Meniere’s disease is unknown. Symptoms of Meniere’s disease appear to be the result of an abnormal amount of fluid (endolymph) in the inner ear, but it isn’t clear what causes that to happen.
Factors that affect the fluid, which might contribute to Meniere’s disease, include:
- Improper fluid drainage, perhaps because of a blockage or anatomic abnormality
- Abnormal immune response
- Viral infection
- Genetic predisposition
Because no single cause has been identified, it’s likely that Meniere’s disease results from a combination of factors.
Symptoms of Meniere’s disease
The symptoms of Meniere’s disease include:
- loss of clear hearing – or loss of ability to distinguish speech or location of sound
- loss of balance (vertigo) – the surroundings seem to spin. Some people feel a degree of motion sickness, while others may even vomit or experience diarrhoea
- noises in the ear (tinnitus) – described as hissing, roaring or ringing, or a combination of sounds. The tinnitus may be relentless, or fade in and out. The volume of the tinnitus is variable too, and often increases before a Meniere’s attack
- hearing loss – usually in the low frequencies and includes a fuzzy, unclear quality to sounds
- ear fullness – a sensation that the ear is under pressure and close to bursting
- sensitivity to noise – some noises can hurt the ears, while other noises may be quiet, but of a particular pitch that causes pain.
Often, one or two symptoms will be more noticeable than others.
Diagnosis of Meniere’s disease
A diagnosis of Meniere’s disease includes vertigo, hearing loss, tinnitus and a feeling of pressure. Many of the symptoms of Meniere’s disease can also be caused by other conditions, so diagnosis of the condition often involves first ruling out other medical possibilities.
There is no specific test for Meniere’s disease, but doctors use a range of tests in combination to help diagnose the disorder. These include:
- Hearing tests – to test if hearing loss is specific to your inner ear. Low frequency loss is an indicator of Meniere’s.
- Electronystagmography (ENG) – measures involuntary eye movement while your balance is put under stress.
- Magnetic resonance imaging (MRI) – can be used to rule out disorders of the central nervous system that may be confused with Meniere’s disease, such as acoustic neuroma, Arnold-Chiari malformation and multiple sclerosis (MS).
Treatment for Meniere’s disease
There is no specific cure for Meniere’s disease. Treatment generally focuses on managing symptoms, and preventing or decreasing the number of attacks. Where possible, the aim is to conserve hearing and reduce balance problems.
Non-surgical options include:
- medication – to control vertigo, nausea and vomiting, and reduce anxiety and fluid retention
- lifestyle changes – stress management, dietary changes, especially a low-salt diet, and quitting smoking
- pressure pulse devices – to help relieve the build-up of pressure and reduce vertigo for people whose symptoms do not respond to medical therapy
- chemical ablation – an antibiotic is used to reduce or destroy the remaining balance (vestibular) functions of the inner ear, so that signals are no longer sent to the brain.
If you are experiencing severe attacks of vertigo and medical treatments don’t help, surgery may be considered as a last resort. This may include procedures that:
- alter the build-up of fluid in your inner ear (endolymphatic sac procedures)
- destroy the balance mechanism of the inner ear (vestibular nerve section or vestibular neurectomy) – these are serious operations that carry a risk of hearing loss, can temporarily disrupt your balance and may require a period of rehabilitation.
Management of Meniere’s disease
Your doctor can help you to find ways to manage your symptoms and help reduce the frequency and severity of attacks associated with Meniere’s disease. Some suggestions include:
- Recognise the warning signs of an attack – sit or lie down immediately when you feel dizzy.
- Rest during and after attacks, before returning to regular activities.
- If you experience balance problems between attacks, you may benefit from doing exercises and activities that help your body and brain regain the ability to process balance information correctly. This is called vestibular rehabilitation therapy.
- Avoid triggers that make your symptoms worse, including sudden movement, bright lights, watching television or reading.
- Beware of losing your balance – good lighting, an even walking surface and use of a walking stick can help you to maintain stability and avoid a fall.
- Avoid driving a car or operating heavy machinery if you experience frequent episodes of vertigo, as this could lead to an accident and injury.
- Use a hearing aid if you experience hearing loss.
- Eat regular meals – an even intake of food and drink throughout the day can help regulate your body fluids.
- Reduce your salt (sodium) intake – eating too much salt increases the fluid in your inner ear and makes your symptoms worse. It is recommended that adults eat no more than 460 mg to 920 mg of sodium (note that one teaspoon of salt contains 2,300 mg of sodium) per day. However, people with Meniere’s are advised to reduce their intake even further to minimise the severity of symptoms. Most fresh foods are naturally low in salt, but processed foods often are not.
- Avoid caffeine and alcohol – excessive amounts of caffeine (in tea, coffee, chocolate and cola drinks) or alcohol can constrict your blood vessels and make your symptoms worse.
- Quit smoking – avoiding nicotine may lessen the severity of your symptoms.
- Join a support group – it can offer understanding and information to help you live with and manage your condition. Your doctor can recommend a support group in your area.
